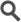Lyme disease is caused by the bacterium Borrelia burgdorferi and is transmitted to humans and animals through the bite of an infected blacklegged tick (Ixodes scapularis). It is found throughout the National Capital Region.
Both the adult and nymphal life stages of the blacklegged tick can transmit Lyme disease when attaching to feed and can be hard to detect due to their small sizes. Adults are approximately the size of a sesame seed, and nymphs the size of a poppy seed (as seen in the image below using a dime as a size reference):

Both people and animals of any age can get Lyme disease. Around 80% of people who are bitten by an infected blacklegged tick will develop symptoms within one to two weeks following a bite. The first symptom is usually a red rash called an erythema migrans (EM) that develops around the bite site. EM starts as small red bump, but slowly expands to up to 12 inches in diameter, and eventually looks like a bulls-eye. It does not itch. Other symptoms in conjunction with the rash often include fever, headache, and fatigue. Weeks to months later, joint pain or facial paralysis may develop. Occasionally the infection can spread to the heart or brain.
In dogs, cats, and horses, the signs of Lyme disease include: joint swelling, shifting leg lameness, fever, lethargy, and swollen lymph nodes. This can progress to kidney disease.
Prevention of tick bites is the best way to protect yourself and your pets from Lyme disease. To learn more about tick prevention and identifying different types of ticks, visit the DC Health tick-borne disease webpage.
If you or a family member has been impacted by Lyme disease and would like to learn more about the disease, please visit the American Lyme Disease Foundation’s website.
Information for Human Healthcare Providers
When treating patients for Lyme disease, keep in mind that ticks can transmit more than one disease, and there is always a potential for coinfection with multiple tick-borne diseases.
Reporting Lyme disease in people
All cases of Lyme disease in a person should be reported within 48 hours of suspected diagnosis or the appearance of symptoms using DC Reporting and Surveillance Center (DCRC), our online reporting system.
The following provides guidance on identifying, testing, and reporting Lyme disease in DC: Lyme Disease Clinical Information, Laboratory Diagnosis, and Reporting for Health Care Providers
Submit Lyme disease reports here, Notifiable Disease and Condition Case Report Form using DCRC.
Diagnosing Lyme disease in people
- Tick-borne Diseases of the US: A Reference Manual for Health Care Providers, Fourth Edition (2017)
- Lyme Disease Rashes and Look-alikes
- Understanding the Immunoblot Test
Treating Lyme disease in people
- The Clinical Assessment, Treatment, and Prevention of Lyme Disease, Human Granulocytic Anaplasmosis, and Babesiosis: Clinical Practice Guidelines by the Infectious Diseases Society of America
- CDC Lyme Disease Treatment Recommendations
- Tickborne Diseases of the US: A Reference Manual for Health Care Providers
Patient handouts and other resources
- European Centre for Disease Prevention and Control Lyme Borreliosis Factsheet for Health Practitioners
- The latest NIH Lyme disease research
Post-Treatment Lyme Disease Syndrome (PTLDS)
It is not uncommon for patients with Lyme disease treated with a recommended 2-4 week antibiotic course to have lingering symptoms of fatigue, pain, or joint and muscle aches when treatment is complete. In a small percentage of cases, symptoms can last more than 6 months. This condition is known as Post-Treatment Lyme Disease Syndrome (PTLDS). Lingering symptoms may be the result of residual damage to tissues and the immune system that occurred during the infection. Similar complications and “auto–immune” responses are known to occur following other infections, including Campylobacter (Guillain-Barre syndrome), Chlamydia (Reiter’s syndrome), and Strep throat (rheumatic heart disease). While the exact cause of PTLDS is unknown what is known is that prolonged use of antibiotics (>4 weeks) does not cure it and can result in serious complications and antimicrobial resistance . While some health care providers claim these symptoms reflect a persistent B. burgdorferi infection “hiding” somewhere in the body leading to “chronic Lyme disease,” there has been no evidence to support this. Several National Institute of Health (NIH) studies have proven prolonged antibiotic use has no benefit, and can have unintended harmful effects.
The following groups DO NOT support the prolonged use of antibiotics to treat Lyme disease:
- American Academy of Neurology
- Centers for Disease Control and Prevention
- Infectious Disease Society of America
More information about complications that can result from prolonged antibiotic use to treat PTLDS can be reviewed in the 2017 CDC MMWR titled Serious Bacterial Infections Acquired During Treatment of Patients Given a Diagnosis of Chronic Lyme Disease — United States.
Information for Animal Healthcare Providers
Reporting Lyme disease in animals
All cases of confirmed Lyme disease in an animal should be reported using DC Reporting and Surveillance Center (DCRC), our online reporting system.
Submit a Lyme disease report for an animal using DCRC.
Lyme disease resources for animal healthcare providers
- Merck Veterinary Manual: Overview of Lyme Borreliosis
- CDC: Preventing Ticks on Your Pets
- Iowa State Center for Food Security and Public Health: Lyme Disease
- Lyme Disease: A Pet Owner's Guide
DC Health Information
For more information on Lyme disease, call (202) 442-9143 or email [email protected].